Replacing An Entire Faulty Gene To Reverse The Blood Disease β-Thalassemia

A team of scientists led by Stanford University researchers Daniel Dever and Matthew Porteus developed a possible gene therapy for the blood disorder β-thalassemia — by replacing an entire gene at once.
β-Thalassemia is a complex condition that can stem from a wide array of mutations of various sizes and types. One of the main underlying problems is a dangerous reduction in the production of haemoglobin, the protein in red blood cells that shuttles oxygen throughout the body, due to a loss-of-function mutation in the HBB gene that produces β-globin. To restore those haemoglobin levels, scientists cut out one of the two HBA genes that produces α-globin and replaced it with a full-length HBB transgene within patient-derived cells in mice, according to the study published last month in the journal Nature Medicine.
About one in 100,000 people develop β-thalassemia, making it one of the more common genetic blood diseases in the world, according to the study. Without adequate haemoglobin to carry oxygen throughout their body, patients often experience symptoms including anaemia, muscle weakness and fatigue. They may also develop enlarged organs and undergo delayed physical development. The reduced haemoglobin levels are rough enough, but the disease is further complicated because only one of the two components of haemoglobin is missing. Without enough β-globin to bind to, excess unpaired α-globin comes out of solution and forms red-blood-cell-killing aggregates that can also lead to blood clots.
Even with recent improvements in how the disorder is treated, patients worldwide have a mean life expectancy of just 30 years.
Extraordinary and promising approach
Unlike sickle cell disease, which is caused by a single point mutation in the HBB gene — and which Graphite Bio and the Stanford Porteus lab tackled in a different recent study — it can be hard to determine the best approach for a β-thalassemia gene therapy given the multitude of contributing mutations, explains Dr Alexis Thompson, the Hematology Section Head at the Ann & Robert H. Lurie Children’s Hospital of Chicago and a professor of paediatrics at Northwestern University's Feinberg School of Medicine. Thompson didn't work on the study and isn't affiliated with its authors, but she said she was encouraged by what the team managed to accomplish.
»The notion of the patient being their own [blood] donor and being able to modify stem cells ex vivo and return them to the patient as a process, that part of it I think we understand,« says Thompson.
»I think now it comes down to the details: what aspects of thalassemia do we actually want to approach? We're able to entertain or imagine these modifications because we are grounded in an approach that I believe is extraordinary and quite promising,« she adds.
A CRISPR gene-editing first
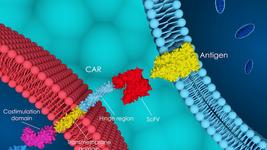
Instead of choosing a specific problem area in the gene to target with a CRISPR Cas9 therapy, the Stanford team decided to swap out the entire gene at once through ex-vivo hematopoietic stem cell transplantation (HSCT): taking out stem cells, swapping an HBA for an HBB gene, and transfusing them into the body, essentially turning patients into their own blood donors.
Replacing an entire gene at once is an incredible scientific feat. In fact, it may well be unprecedented* across the entire gene editing field, says study author Daniel Dever, now the co-founder and head of discovery research at the San Francisco-based gene-editing company Graphite Bio.
But aside from bragging rights, the accomplishment allowed the researchers to simultaneously downregulate α-globin and upregulate β-globin so that the two were produced at a healthy balance.
»We had this idea: What if you could overexpress β-globin through the α-globin promoter? It would potentially kill two birds with one stone. It would simultaneously reduce the expression of α-globin and increase expression of b-globin,« says Dever.
»We were able to show that it decreases alpha while it increases beta. That was the goal we were looking for,« he adds.
In theory, the team could have tried to swap out the HBB gene for a functional version, but targeting one of the HBA genes makes more sense for a variety of reasons, Dever explains. Chief among them is the fact that β-thalassemia is a complex disease caused by various mutations, some patients may still have residual, endogenous β-globin production, and it would be counterproductive to knock that out.
Thompson says that β-thalassemia could be considered a manageable chronic disease thanks to improvements in both blood-iron level monitoring techniques and the overall safety of the blood supply. But a curative approach through gene therapy, she suggests, would revolutionize the field — and could be ready in the next few years.
Turning gene-swapping into a cure

The big question, of course, is whether the corrective effects in individual cells and mouse models translate into curative effects for human patients.
»Creating these humanized models in the mouse setting eventually runs up against the realities that there are distinct differences [between mice and people]. At some point, the issue becomes being able to take this proof of concept that's been done so elegantly in these various mouse models and establish that something similar can be achieved when in human cells. And then the next question in the thalassemia patient is 'Can you do this at scale?' Can you do these corrections, avoiding increases in indels, and get them to a level where they're making sufficient haemoglobin in a human to perhaps render them transfusion independent?« says Thompson.
There's reason to suspect it might work — at least more reason to think so than for the other gene therapy approaches that have been floated for β-thalassemia — but it's far too soon to tell.
That's because replacing HBA1 with HBB, using the α-globin promoter to produce β-globin, while leaving HBA2 alone so it can continue to produce α-globin, theoretically stands to rebalance globin levels in a way that other approaches don't. Scientists previously suggested using CRISPR Cas9 to reawaken the fetal precursor to β-globin to make up for low haemoglobin levels. But with both HBA1 and HBA2 in full swing, there could still be dangerous levels of unpaired α-globin that the fetal globin approach couldn't account for.
This is the same decision that Graphite Bio made when developing a possible treatment for Sickle Cell Disease. In both cases, Porteus and his team decided to address the mutation directly rather than rely on upregulated fetal globin to make up the difference. Dever says that the team at Graphite Bio hasn't yet decided whether they want to pursue the β-thalassemia gene therapyfurther. But if they do, the ability to replace an entire gene in a clinical setting would represent a potential paradigm shift in how blood disorders are treated.
“this would be a remarkable advancement for a curative approach in thalassemia”Alexis Thompson
»I think that to be able to put together a series of experiments that are as elegant as the ones that they’ve laid out, with the results that they have, is extremely impressive and very encouraging. That is different than saying that we're ready to do this in a person. But if this were effective, this would be a remarkable advancement for a curative approach in thalassemia,« says Thompson.
Opens the door to replacing large DNA segments
Even if the gene therapy doesn't pan out in a clinical setting, this paper stands to be incredibly impactful for the gene-editing field. It presents a rare instance where the methodology might end up being just as important for researchers as the outcome is for doctors.
The unprecedented success at swapping out an entire gene — a new concept that the Graphite Bio team is calling Total Gene Replacement — is such an ambitious endeavour that Dever says he wasn't even sure it would work.
The challenge — aside from the logistical hurdle of transporting such a long stretch of DNA — is that both HBA genes are genetically identical. Any CRISPR Cas9 vector that cuts one would also cut the other, introducing the possibility of multiple double-strand breaks or other serious errors, Dever explains.
The team had to find sequences in the stretch of DNA between HBA1 and HBA2 that were different so that they could make cuts there, specifically targeting just one gene over the other.
»That brought up another interesting conundrum. Normally what you try to do is target closer to the start of the gene so that you can use the endogenous promoter to drive the expression of the gene. But in this case, we were at the end of the gene because that's where HBA1 and HBA2 differ enough to identify a specific Cas9 site. So, to test that, we thought, 'Well, what if we could make a double-strand break at the end of the gene and use one homologous arm at the front of the gene and another homologous arm at the end of the gene?',« Dever says.
That precision, the ability to cut out one HBA gene without affecting the other, is what makes this study and approach so elegant, as Thompson describes it.
»Being able to target only a single HBA allele, I think, is essential. Being sure that the targeting is such that the disruption is that specific — I think that's very important. Being able to move that big a piece of DNA was just quite impressive,« Thompson says.
»The danger would be of converting someone from β-thalassemia to having α-thalassemia as well. But they clearly were able to demonstrate being able to identify the guide that had the high-frequency cutting that would allow them to target only one of them,« she adds.
Therapeutically relevant for other conditions
It was a long shot, Dever admits, but being able to use the α-globin promoter, one of the strongest in the human body, to restore β-globin production to healthy levels, was too good of an opportunity to pass up.
»To our surprise, it worked very well. We can preserve the α-globin and red blood cell-specific expression,« Dever says.
»We thought that was a novel finding. A mechanism of action through which we were able to replace an entire gene — and replace that gene with a therapeutic gene at the same time.«
By doing so, he thinks, the team may have uncovered a new way to approach gene therapies. If the Total Gene Replacement approach works with other genes, Dever says that researchers may be able to use red blood cells to ferry proteins throughout the body to treat other genetic conditions.
»There's some astronomical number of red blood cells you make in a day. To be able to take advantage of the lifespan and mass production of red blood cells would be an exciting way to deliver proteins throughout the body,« Devers says.
»We're interested in the potential of using the platform for new treatments for these conditions,« he adds.
Of course, the Total Gene Replacement approach won't be appropriate for every genetic condition. β-Thalassemia is a unique case because there are two HBA genes, and replacing one of them happens to rebalance the α-globin versus β-globin equation. The numbers might not work out right for other conditions or diseases, and Dever says they'll have to proceed on a very cautious, case-by-case basis.
»Picking an indication has to be based on the fact that current therapies aren't efficacious or they're unsafe. It has to be a disease that's not addressable right now, and there's a patient population and market where Graphite can make a substantial benefit to human health,« says Dever.
Link to original article in Nature Medicine: Gene replacement of α-globin with β-globin restores hemoglobin balance in β-thalassemia-derived hematopoietic stem and progenitor cells.
* [Update: Mario Amendola's group at Université Paris Saclay, France published the same strategy (same cells and gene) one month prior].
Dan Robitzski is a science journalist and former neuroscientist based in Los Angeles.
Tags
ArticleInterviewNewsin vivoBeta ThalassemiaRare DiseaseGene therapyCRISPR-CasCas9
CLINICAL TRIALS
Sponsors:
Wave Life Sciences Ltd.